Why nighttime urination, urgency, weak stream, and incomplete emptying may be more than “just getting older.”

Nighttime urination can quietly disrupt sleep, energy, and quality of life.
It usually does not happen all at once.
First, you notice you are standing at the toilet a little longer. Then you start getting up once at night. Then twice. Then three times. Maybe your stream is weaker than it used to be. Maybe you start looking for bathrooms before meetings, movies, road trips, or golf rounds.
At first, it is easy to shrug it off.
“I’m just getting older.”
“I drink too much coffee.”
“It’s annoying, but I can live with it.”
And sometimes, that is true. Mild urinary symptoms may simply require monitoring. But when symptoms from an enlarged prostate begin affecting sleep, daily routines, energy, travel, exercise, or bladder emptying, they deserve a closer look.
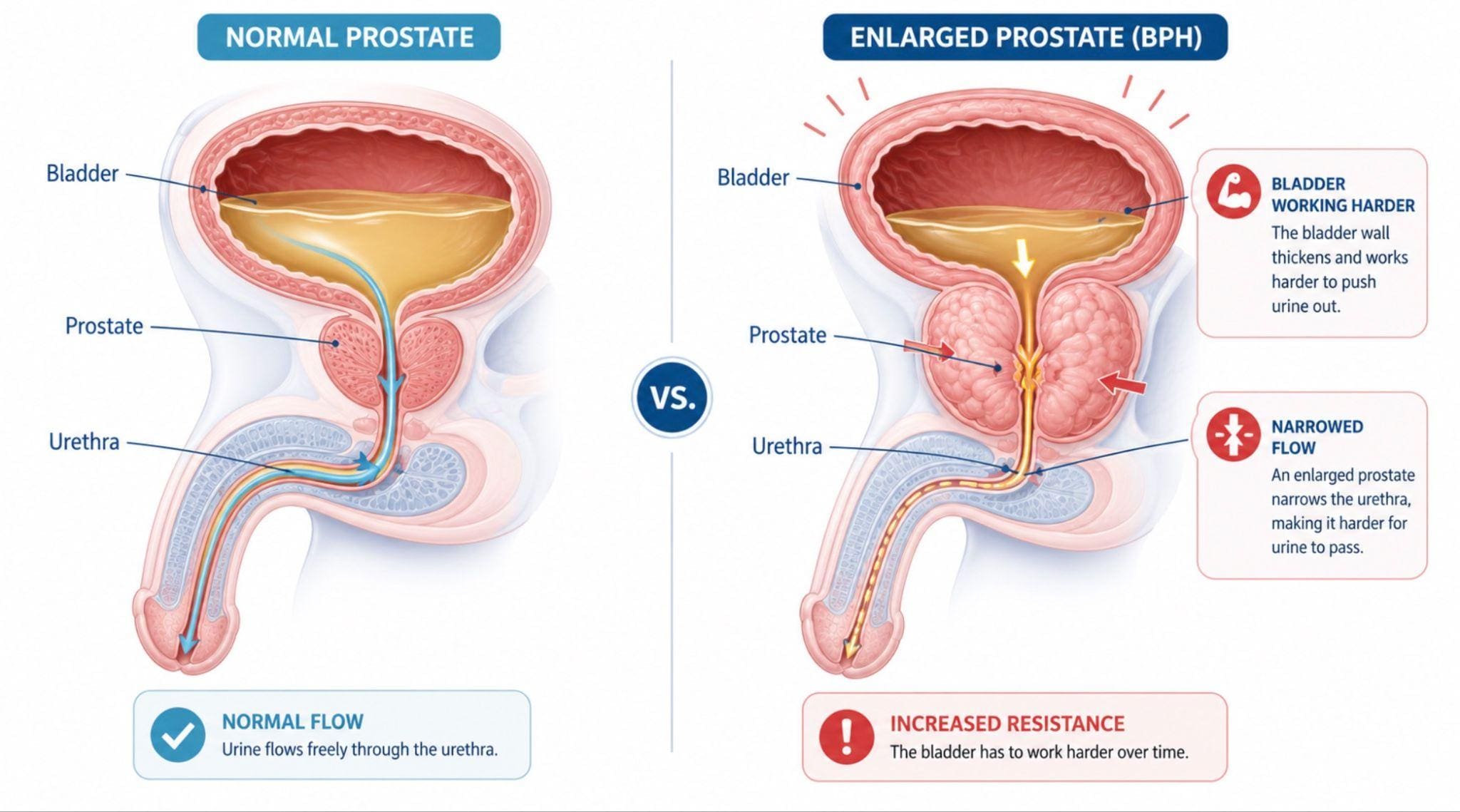
BPH, or benign prostatic hyperplasia, is a non-cancerous enlargement of the prostate. It is extremely common as men get older. The prostate surrounds the urinary channel, so as it enlarges, it can contribute to symptoms such as a weak stream, urgency, frequency, nighttime urination, hesitancy, and incomplete emptying.
The question is not whether every man with BPH symptoms needs treatment.
The better question is this:
Are your symptoms still mild and manageable, or are they quietly changing how you live?
Men Are Good at Adapting
One reason BPH symptoms get ignored is that men adapt.
They stop drinking water before leaving the house. They sit near the aisle at the movie theater. They avoid long drives. They scan restaurants for the restroom. They wake up tired but blame work, stress, age, or a bad mattress.
Over time, the new routine starts to feel normal.
But urinary symptoms can take more from your life than you realize. Getting up several times a night can leave you exhausted the next day. Urgency can make meetings stressful. Frequency can interrupt work, exercise, sleep, intimacy, and social activities. A weak stream or incomplete emptying can turn something simple into a daily frustration.
And sometimes, the problem announces itself more dramatically. A man may suddenly find that he cannot urinate at all. That can lead to an emergency room visit and catheter placement, often at the worst possible time.
“Some men come in because their symptoms are slowly taking over their lives. Others come in after they suddenly cannot urinate and end up with a catheter in the emergency room, often in the middle of the night or over the weekend,” says Dr. Rich Bevan-Thomas, urologist with Urology Partners of North Texas. “In simple terms, that is the day the bladder lost the battle against the prostate. At that point, we need to evaluate why the bladder could not empty and what we can do to improve the chances of successful urination going forward.”
BPH symptoms are not just bathroom symptoms. They can become lifestyle symptoms. And in some men, they can eventually become urgent medical problems.
The issue is not just how often you urinate. The issue is whether your bladder is starting to run your schedule or struggling to keep up.
Urgency and Frequency May Be Bladder Symptoms Too
Many men think BPH only causes a weak stream. But men with BPH can also develop urgency, frequency, and nighttime urination. These are sometimes called storage symptoms because they involve how the bladder stores urine, not just how urine flows out.
This is where overactive bladder, or OAB, enters the conversation.
OAB can happen in men without an enlarged prostate. It can also be related to other bladder, neurologic, or medical issues. But in men with BPH, urgency and frequency often overlap with prostate enlargement because the bladder may become more sensitive, irritated, or overworked over time.
That is why it is not enough to say, “I only have urgency, so it must not be my prostate,” or “I only have frequency, so I’ll just drink less water.”
Sometimes urgency and frequency are bladder-driven. Sometimes they are prostate-driven. Often, in men, the prostate and bladder are both part of the story.
“Men often think about BPH as a weak-stream problem, but urgency and frequency can be just as disruptive,” says Dr. Tony Mammen, urologist with Urology Partners of North Texas. “The bladder and prostate work together, so evaluation helps us understand whether symptoms are mainly coming from prostate enlargement, bladder overactivity, or a combination of both.”
Nighttime Urination Is Not Just Annoying
Nocturia means waking up at night to urinate. For some men, getting up once is not a major problem. But getting up two, three, or four times a night can fragment sleep and make it harder to function the next day.
Sleep is not optional maintenance. It is part of health.
That does not mean BPH directly causes fatigue, weight gain, low testosterone, mood changes, or cognitive decline. But if urinary symptoms repeatedly disrupt your sleep, the sleep disruption itself may become a real health issue.
The cost is often subtle at first. You are a little more tired. You skip the gym. You snack more. You move less. You feel less sharp. You have less patience. You are not quite yourself.
Over months and years, that matters.
Poor sleep can make it harder to maintain weight and energy. There is also evidence that sleep restriction can affect testosterone. That does not mean every man waking up at night has low testosterone because of BPH. It means sleep quality should be taken seriously when men are concerned about energy, strength, libido, and overall vitality.
There is also growing interest in the relationship between sleep and brain health. Again, the point is not that waking up to urinate causes dementia. The point is that chronic sleep disruption is not something men should casually ignore.
“When a man is getting up three or four times a night, we should not treat that as a minor inconvenience,” says Dr. Geoffrey Nuss, urologist with Urology Partners of North Texas. “That kind of sleep disruption can affect energy, mood, weight, exercise, and quality of life. The goal is not to scare patients. The goal is to help them recognize when symptoms are worth measuring and evaluating.”
BPH Can Shrink Your World
Some BPH symptoms are easy to measure. How many times did you get up last night? How often do you urinate during the day? How weak is your stream?
Other effects are harder to notice because they happen gradually.
A man may stop going to movies because he does not want to climb over people twice. He may avoid long meetings because he worries about urgency. He may plan road trips around bathrooms. He may drink less water during the day to avoid frequency, then feel dehydrated or fatigued. He may avoid exercise because urgency makes it inconvenient.

BPH symptoms can gradually change how men travel, work, exercise, and socialize.
None of this sounds dramatic.
But it is still a loss of freedom.
That is one of the most important reasons BPH symptoms matter. They can quietly make a man’s life smaller.
The Bladder Matters Too
BPH is often described as a prostate problem, but the bladder is a major part of the story.
As the prostate enlarges, the bladder may have to work harder to push urine through a narrowed channel.
When the prostate makes urination more difficult, the bladder has to generate more pressure to push urine out. For a while, the bladder can often compensate. It may work harder, squeeze stronger, and still empty reasonably well.
But compensation is not the same as health.
Over time, a bladder that constantly works against resistance can begin to change. The bladder wall may become thicker and less flexible. Some men experience increased urgency and frequency because the bladder becomes irritated or less able to comfortably store urine. Others may begin retaining more urine because the bladder muscle becomes tired or weaker.
In simple terms, the bladder can only compensate for so long.
In more advanced cases, the bladder can stretch due to chronic, incomplete emptying. When that happens, it may lose some of its natural elasticity and squeezing power. If the bladder becomes overstretched for too long, some men may develop long-term bladder dysfunction. That means even if the prostate problem is later treated, the bladder may not fully recover its ability to empty normally.
This is one of the most important reasons not to ignore worsening symptoms forever.
The bladder can compensate for a while. But if it keeps fighting the prostate year after year, it may eventually lose strength, flexibility, and function.
This does not mean that every man with mild urinary symptoms is at risk. But there are real consequences when symptoms are progressive, severe, or associated with incomplete emptying, retention, infections, bladder stones, or kidney problems.
“The earlier we understand what is happening, the more options patients usually have,” says Dr. Keith Xavier, urologist with Urology Partners of North Texas. “Evaluation does not automatically mean treatment. Sometimes it simply means getting a clearer picture of symptom severity, bladder emptying, and prostate health.”
That is the point patients need to understand. A man may still be urinating, but that does not always mean his bladder is emptying well or working efficiently.
Stop Guessing: Use an IPSS Score
One of the simplest ways to take urinary symptoms seriously without overreacting is to measure them.
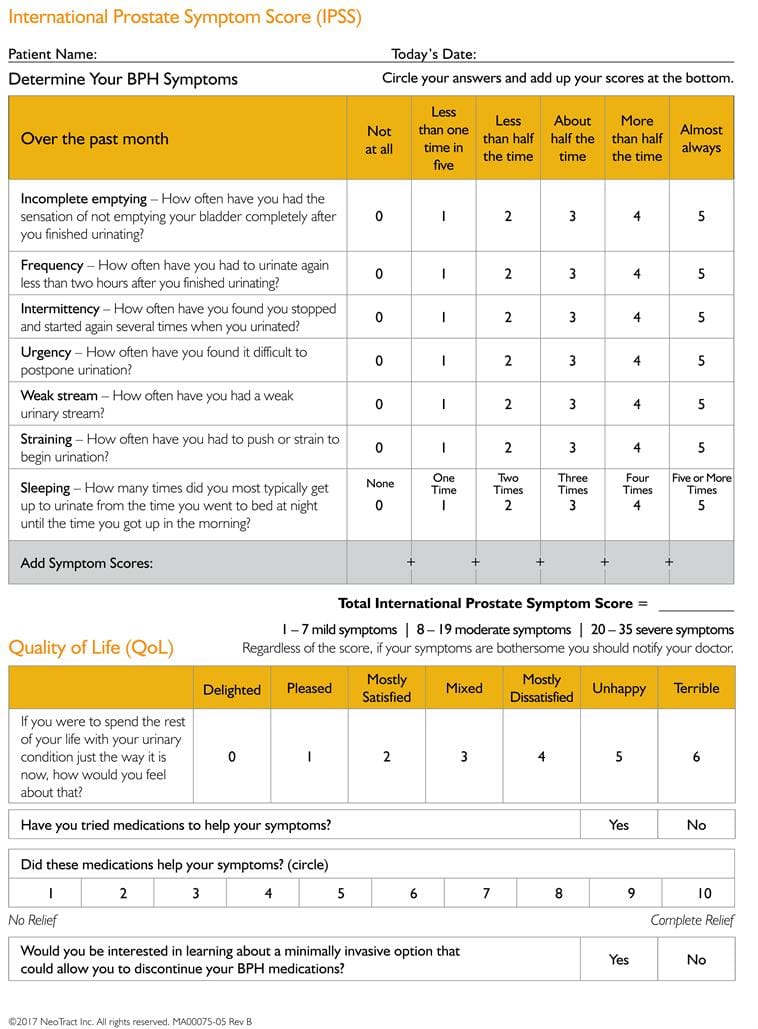
The International Prostate Symptom Score, also called the IPSS or AUA Symptom Index, is a short questionnaire used to assess urinary symptoms commonly associated with BPH. It asks about incomplete emptying, frequency, intermittency, urgency, weak stream, straining, and nighttime urination. It also includes a quality-of-life question.
This matters because men often underestimate their symptoms.
A man may say, “I’m doing fine,” but his answers show that he urinates every one to two hours, wakes up three times a night, frequently has urgency, and often feels incomplete emptying.
That is not “fine.” That is a measurable pattern.
In general, an IPSS score of 0–7 is considered mild, 8–19 is moderate, and 20–35 is severe. If your score is 8 or higher, or if symptoms such as nighttime urination, urgency, frequency, weak stream, or incomplete emptying are bothering you, it may be time to schedule an evaluation. The number matters, but so does the impact on your life.
Using an IPSS score helps turn a vague feeling into something more objective. It also helps track whether symptoms are stable, improving, or getting worse.
That can be especially useful for men who want to start with lifestyle changes. Instead of guessing whether things are better, they can repeat the questionnaire several weeks later and compare.
When Is It Time to See a Urologist?
A urology evaluation does not automatically mean medication or a procedure. Often, it simply helps answer a few important questions.
How severe are the symptoms? Is the bladder emptying well? Is the prostate likely contributing? Are there signs of infection, blood, retention, or other concerns? Are symptoms mild enough to watch, or significant enough to treat?
Men should consider evaluation when symptoms persist, worsen, or interfere with sleep, work, travel, exercise, meetings, movies, intimacy, or daily life.
They should be evaluated sooner if they have blood in the urine, recurrent urinary tract infections, bladder stones, urinary retention, concerns about kidney function, or a strong sensation of incomplete emptying.
The goal is not to push every man toward treatment.
The goal is to stop guessing.
What Comes Next?
Once a man understands that BPH symptoms matter, the next question is practical:
“What can I do about it?”
Some men start with lifestyle changes. Some try over-the-counter prostate supplements. Others may benefit from prescription medications. And for men who do not get enough relief from pills, or who do not want to stay on medication long-term, minimally invasive and surgical options may be considered.
In next week’s UPNT article, we will take a closer look at over-the-counter prostate supplements, a multibillion-dollar industry built around men looking for relief from urinary symptoms. We will discuss why these products are so appealing, what the evidence actually shows, and how men can tell whether a supplement is truly helping or simply offering hope in a bottle.
Future UPNT articles will also discuss prescription medications for BPH and minimally invasive treatment options.
The most important step is understanding where you are now.
Are your symptoms mild and stable? Are they slowly getting worse? Are they disrupting sleep? Are they changing how you travel, work, exercise, or socialize? Are you emptying well?
Those answers matter.
The Bottom Line
BPH symptoms are common, but that does not mean they should always be ignored.
If urinary symptoms are mild, stable, and not affecting quality of life, observation may be reasonable. But if your IPSS score is 8 or higher, or if you are waking up several times a night, struggling with urgency, avoiding activities, sitting near exits, leaving movies or meetings, or feeling like your bladder is running your schedule, it may be time to take the symptoms more seriously.
At Urology Partners of North Texas, our physicians help men understand their urinary symptoms, measure severity, evaluate bladder emptying, and review treatment options based on each patient’s goals.
The goal is not to scare you into treatment.
The goal is to help you stop adjusting your life around your bladder.
If your IPSS score is 8 or higher, or if urinary symptoms are affecting your sleep, energy, routine, or quality of life, schedule an appointment online with a UPNT urologist. A proper evaluation can help identify what is driving your symptoms and create a better game plan.